The “Proposed Indication” for Multikine
that will be submitted to the FDA in a license application will be
limited by certain eligibility criteria to patients who would be
deemed by NCCN Guidelines as having a lower risk for tumor
recurrence. The Standard of Care for lower risk for tumor
recurrence advanced primary head and neck cancer patients is
surgery followed by radiotherapy, but not chemotherapy. Note
that the term “lower risk for recurrence” should not be confused
with a low risk of death, because the 5-year survival for such
patients is still less than 50%, even after receiving the current
standard of care (SOC). The Proposed Indication for Multikine would
cover an estimated 210,000 patients globally each year.
Data collected during the Phase 3 trial that will be submitted
to FDA in support of the Proposed Indication are:
- Partial and complete tumor responses
within 3 weeks and before surgery (objective responses per
RECIST):
- 8.1% (32/395) objective response rate (ORR) for Multikine+CIZ
patients in the intent-to-treat (ITT) population versus zero in the
SOC group (n=394).
- 15.2% (24/158) ORR for Multikine+CIZ patients in the
lower-risk-for-recurrence arm versus zero in the SOC group
(n=168).
- Two-sided Fisher Exact p-values <0.0000001 for ORR.
- Complete responses before surgery were seen in 5 Multikine+CIZ
patients.
- Objective response before surgery was
prognostic/predictive of improved overall survival (OS) and
significant for reduced death rate:
- In the ITT population, 22.2% death rate versus 54.1% death rate
(Multikine objective responders versus Multikine non-responders;
two-sided Fisher Exact p-value <0.0001; HR=0.301 [95% CI 0.16,
0.566]).
- In the lower-risk-for-recurrence arm, 12.5% death rate versus
41.0% death rate (Multikine+CIZ objective responders versus
Multikine+CIZ non-responders; two-sided Fisher Exact
p-value=0.0101; HR=0.246 [95% CI 0.077, 0.787]).
Data that will be provided to FDA to confirm efficacy in the
Proposed Indication:
- Analysis of the lower-risk-for-recurrence
arm was pre-specified in the original study protocol and in
the statistical analysis plan. This arm comprised about 40% of all
study participants.
- 14.1% absolute OS advantage at
5-years in the lower-risk-for-recurrence arm (62.7% vs
48.6%) for Multikine+CIZ patients versus SOC patients. OS benefit
was also shown at 1, 2, 3, and 4 years.
- Nearly 4-year increase in median overall
survival in the lower-risk-for-recurrence arm (101.7 months
for Multikine+CIZ versus 55.2 months for the SOC).
- Histopathological analysis confirmed the
effect of Multikine, as 61 markers, ratios, and combinations
showed a statistically significant effect in the
lower-risk-for-recurrence arm (two-sided p<0.05) favoring
Multikine+CIZ versus the SOC for OS, progression free survival, and
loco-regional control outcomes.
- Additional (confirmatory)
progression-free survival benefit in the
lower-risk-for-recurrence arm was observed for Multikine+CIZ versus
the SOC.
- No excess safety issues: The
overall incidence of adverse events and serious adverse events in
the Multikine arms was not substantially different versus the
SOC.
The pivotal Phase 3 trial is intended to support a Biologics
Licensing Application to FDA, which has not yet been submitted. FDA
is the only U.S. entity authorized to determine safety and
efficacy. Multikine is currently not FDA approved.
CEL-SCI Corporation (NYSE American: CVM) announced today
that the results of its 10-year IT-MATTERS pivotal Phase 3 clinical
trial in head and neck cancer with its investigational
immunotherapy Multikine®* (Leukocyte Interleukin, Injection) have
been posted on clinicaltrials.gov per U.S. government requirements.
(See
https://clinicaltrials.gov/ct2/show/results/NCT01265849?term=multikine&draw=2&rank=2).
Clinicaltrials.gov is the largest clinical trial database in the
world. It is run by the U.S. National Library of Medicine at the
National Institutes of Health. Some of the trial’s results were
published in two peer-reviewed abstracts and a poster at the ASCO
conference in June 2022. (See
https://www.businesswire.com/news/home/20220527005092/en/.)
Additional results will be published in scientific journals and
presented in scientific forums in the future.
Design of IT-MATTERS Phase 3 Trial
The 928-patient IT-MATTERS study was designed to determine if
Multikine provided survival and other clinical benefits to patients
suffering from locally advanced primary squamous cell carcinoma of
the head and neck (SCCHN), oral cavity and soft-palate. Multikine
is a mixture of naturally occurring cytokines that regulate the
immune system. Multikine is the first investigational cancer
immunotherapy being developed as a first-line neo-adjuvant
treatment to be provided to previously
untreated locally advanced primary disease SCCHN patients
before they receive the SOC. The
global IT-MATTERS trial was conducted in 23 countries in accordance
with Good Clinical Practices, International Counsel for
Harmonization standards, and all other country-specific regulatory
requirements.
Following diagnosis, subjects were randomized into one of three
treatment arms. In the primary treatment arm (3/7) subjects
received three consecutive weeks of treatment with supraphysiologic
doses of Multikine injected 5x/wk peritumorally and
perilymphatically plus “CIZ” prior to receiving the SOC. (CIZ
comprised a non-chemotherapeutic dose of cyclophosphamide
(administered one-time only IV-bolus, 3 days prior to the 1st dose
of Multikine), and indomethacin and zinc-multivitamins daily from
day 1 of Multikine administration to one day before surgery to
enhance Multikine activity.) In the second arm (1/7), subjects
received the three-week Multikine regimen without CIZ prior to
receiving the SOC. In the third arm (3/7), which was study control
arm, subjects received only the SOC (with no Multikine or CIZ).
Thus, all subjects in the study received the SOC, but some subjects
received Multikine before the SOC (the two study treatment arms)
and some did not (study control arm). The two main comparator
groups in the study were the primary arm (Multikine+CIZ+SOC) and
the study control arm (SOC alone).
The SOC for all research subjects was identical and involved a
bifurcated treatment path following surgery, i.e., a
radiotherapy-only arm and a concurrent chemoradiotherapy arm. To
determine which path a patient should take, the treating physicians
decided after surgery based on pathology and medical judgment, as
guided by the National Comprehensive Cancer Network (NCCN)
Guidelines, whether the patient was at a higher risk for tumor
recurrence. These patients would receive concurrent
chemoradiotherapy. All other patients were classified as lower risk
for recurrence and would receive only radiotherapy after
surgery.
The “Proposed Indication” for Multikine will be limited by
certain eligibility criteria to select patients deemed by NCCN
Guidelines for the lower-risk-for-recurrence group. Patients would
not meet the eligibility criteria if they present with adverse
features that would place them in the higher-risk-for-recurrence
group per NCCN Guidelines. Note that the term “lower risk for
recurrence” should not be confused with a low risk of death,
because the 5-year survival for such patients is still less than
50%, even after receiving the current SOC.
It must also be noted that the bifurcated treatment path
described above was not created by CEL-SCI for its study but was,
and still is, the SOC per NCCN Guidelines for advanced primary
SCCHN patients. Because it would have been unethical to deprive any
subjects of the SOC, the only ethical way to have conducted the
study was to use the bifurcated SOC following surgery—it would not
have been ethically permissible to study Multikine in only one
treatment arm at a time (lower-risk or higher-risk only).
Furthermore, because it was obvious when the study was designed
that Multikine might provide a benefit in only one of the two SOC
risk groups, CEL-SCI pre-specified in its original study protocol
that analyses of the trial results should take place for all, as
well as for each of these groups. Separate analyses of the
lower-risk-for-recurrence and higher-risk-for-recurrence treatment
arms were also pre-specified in the study’s statistical analysis
plan which was completed before data lock and the study result were
analyzed.
About 40% of study subjects (n=380) were classified and met the
NCCN requirements for having a lower risk of tumor recurrence, and
it was in this arm of the study that the vast majority of the
objective responders discussed above were observed. It was also
observed in this arm that Multikine+CIZ-treated non-responders
still saw OS benefit. Thus, when the lower-risk-for-recurrence arm
was viewed as a whole (responders plus non-responders together), a
statistically significant OS benefit from Multikine was observed
overall, which provided a nearly four-year
extension of median survival time versus the control.
Using data from the study, CEL-SCI developed eligibility
criteria to select, prior to surgery, the patients who would be
slated for classification by the NCCN Guidelines as
lower-risk-for-recurrence. This distinction currently can be
determined only after surgery. Based on the ability to select
subjects before surgery who should receive the Multikine treatment,
CEL-SCI plans to seek FDA approval for the treatment of locally
advanced primary disease SCCHN subjects who would receive Multikine
first, then receive surgery, and then receive only radiotherapy,
per NCCN Guidelines.
The Proposed Indication represents about 210,000 patients
worldwide per year. To CEL-SCI’s knowledge the last medical advance
for such patients impacting their overall survival occurred when
Methotrexate was approved over 60 years ago. Multikine also
received FDA Orphan Drug Designation for the “neoadjuvant therapy
in patients with squamous cell carcinoma of the head and neck
(SCCHN).” There is thus a clear unmet medical need for improved
treatments for these patients.
IT-MATTERS Phase 3 Trial Results Summary
This release summarizes the results recently posted on
clinicaltrials.gov for the overall ITT population as well as the
subjects constituting the Proposed Indication representing 41.2% of
the study overall ITT population. (See
https://clinicaltrials.gov/ct2/show/results/NCT01265849?term=multikine&draw=2&rank=2)
Please refer to the clinicaltrials.gov presentation of the data for
further information on study design and study data.
- Objective Responses Before Surgery
(partial and complete tumor response per RECIST, confirmed at
surgery by pathology): In the overall ITT population,
objective responses before surgery (sometimes also called “early
responses”) were observed in 45 subjects who received Multikine for
3 weeks; no such responses were observed in the SOC alone (control)
(p<0.00000001).
- Five subjects who received Multikine+CIZ had complete tumor
responses confirmed at surgery.
- In the overall ITT population (n=923), objective responses were
seen in:
- 8.5% of Multikine-treated subjects (45/529).
- 8.1% of the Multikine+CIZ treatment arm (32/395).
- 9.7% of the Multikine without CIZ treatment arm (13/134);
- 0% of the SOC alone (control) treatment arm (0/394).
- In the Proposed Indication (n=380), objective responses were
seen in:
- 16.0% of Multikine-treated subjects (34/212).
- 15.2% of the Multikine+CIZ treatment arm (24/158).
- 18.5% of the Multikine without CIZ treatment arm (10/54);
and
- 0% of the SOC alone (control) treatment arm (0/168).
- Objective Responses Before Surgery Were
Prognostic For Survival with a
Significant Decrease in Death Rate:
- In the overall ITT population (n=923), the 22.2% death rate
among Multikine objective responders before surgery (n=45) was
significantly lower (two-sided Fisher Exact test p<0.0001;
HR=0.301) than the 54.1% death rate for the remaining Multikine
non-responders (n=484);
- In the Proposed Indication (n=380):
- the 17.6% death rate among all Multikine objective responders
before surgery (n=34) was significantly lower (two-sided Fisher
Exact test p=0.0067; HR=0.348) than the 42.7% death rate for the
remaining Multikine non-responders (n=178).
- the 12.5% death rate among Multikine+CIZ objective responders
before surgery (n=24) was significantly lower (two-sided Fisher
Exact test p=0.0101; HR=0.246) than the 41.0% death rate for the
remaining Multikine non-responders (n=134).
- Significant OS advantage in the Proposed
Indication for the Multikine+CIZ treatment arm versus the
SOC control:
- 5-year absolute OS advantage of 14.1% (62.7% vs 48.6%);
- proportional hazards two-sided p=0.0236;
- 0.68 hazard ratio equating to a 47% OS prolongation; and
- 3-year and 4-year absolute OS advantage of 4.9% and 9.5%,
respectively, are supportive.
- In the overall ITT population, no statistically significant OS
difference was seen between the two main comparator groups
(proportional hazards two-sided p=0.4128). It is believed that the
higher-risk-for-recurrence patients in the overall ITT were too
sick to tolerate the extra three-weeks before surgery for the
Multikine treatment and also that chemotherapy may impair
Multikine’s immunological mechanism of action.
- Nearly Four-Year Median OS
Benefit: In the Proposed Indication, the median OS for those
receiving Multikine+CIZ was 101.7 months versus 55.2 months for the
control, a survival improvement of almost four years. The Multikine
treatment arm without CIZ in the Proposed Indication also had
better median OS than control (68.2 months vs. 55.2 months).
- Progression-Free Survival (PFS):
In the Proposed Indication, there was confirmatory PFS difference
between the two main comparator groups (HR=0.76; proportional
hazards two-sided p=0.0896). In the overall ITT population, there
was no statistically significant PFS difference between the two
main comparator groups (proportional hazards two-sided
p=0.3728).
- Locoregional Control (LRC): In the
Proposed Indication, there was no statistically significant LRC
difference between the two main study groups (proportional hazards
two-sided p=0.4082). In the overall ITT population, there was no
statistically significant LRC difference between the two main
comparator groups (proportional hazards two-sided p=0.8020).
- Significant Histopathological
Results: OS, PFS, and LRC were examined using a proportional
hazards model to assess the interactions between histopathology
(HP) cellular marker expression levels, risk group (lower and
higher), and treatment in the two main comparator groups. Twenty HP
markers were classified as low, medium, and high. Two HP ratios
were classified as low, medium, and high. Fourteen HP combinations
were classified as low and high. These resulted in 94 possible
comparisons for each of OS, PFS, and LRC. Significance favoring
Multikine+CIZ vs. control (two-sided p<0.05) was observed in the
Proposed Indication as follows:
- OS: 14 markers, 2 ratios, and 9 combinations;
- PFS: 11 markers, 1 ratio, and 5 combinations;
- LRC: 9 markers, 1 ratio, and 6 combinations;
- Combined (summed across endpoints), significance was reached
for 21.6% (61/282) of the total possible comparisons, and the
one-sided 97.5% confidence bound on the fraction significance was
16.3% which exceeds 5% chance alone.
- No excess safety issues:
- The overall adverse event rates were 92.4% for the
Multikine+CIZ treatment arm; 95.9% for the treatment arm receiving
Multikine without CIZ, and 96.1% for the SOC alone (control)
treatment arm.
- The overall serious adverse event rates were 53% for the
Multikine+CIZ treatment arm, 50.7% for the treatment arm receiving
Multikine without CIZ, and 52.7% for the SOC alone (control)
treatment arm.
- The incidence of adverse events and serious adverse events
noted in the Multikine arms was not substantially different from
those in control.
Importance of Multikine’s IT-MATTERS Trial Results
Head and neck carcinomas constitute about 890,000 cases annually
worldwide. In the United States, there are about 68,000 new cases
annually. Of those, 90% are squamous cell carcinomas, and
approximately two-thirds of these patients present on their first
visit with locally advanced primary (untreated) disease. Currently,
the median 3-year OS with the existing SOC is estimated at 55%. The
5-year OS is approximately 43%. There are clearly many locally
advanced primary SCCHN patients who are not well served by the
currently available treatment modalities.
The IT-MATTERS trial confirms that a 3-week treatment with
Multikine provides objective responses before surgery with
statistically significant five-year OS benefit for the Proposed
Indication, i.e., patients deemed by the NCCN Guidelines as lower
risk of recurrence and who should receive radiotherapy without
chemotherapy following surgery.
Multikine administration (+/- CIZ), as the first therapy after
diagnosis, demonstrated objective complete and partial responses
before surgery in 8.5% of the overall ITT population and in 16.0%
of all Multikine-treated patients (+/- CIZ) in the
lower-risk-for-recurrence treatment arm. A partial response means
that the tumor has been reduced by at least 30%, and a complete
response means that the tumor has completely disappeared. These
objective tumor responses were noted within three-weeks of the
beginning of Multikine treatment up to surgery and provided direct
evidence of Multikine’s anticancer activity.
Although objective responses to cancer drugs do not always lead
to improved survival, in the case of Multikine, objective responses
resulted in a significantly reduced death rate. For Multikine+CIZ
patients in the Proposed Indication, the death rate fell from 41%
for non-responders to 12.5% for objective responders. A similar
effect was also seen for objective responders in the overall ITT as
well.
These reduced death rates yielded an absolute OS advantage of
14.1% at 5-years versus the SOC alone in the
lower-risk-for-recurrence treatment arm, with a proportional hazard
p-value of 0.0236, a hazard ratio of 0.68 (representing 47%
prolongation of survival), a median overall survival that is nearly
4-years longer than from the SOC alone, confirmatory PFS benefit,
and histopathological data showing the direct effect of the
Multikine treatment on the tumor and the tumor
microenvironment.
These statistics mean that for every 100 patients who would
receive Multikine (if approved) followed by surgery and
radiotherapy only, the likelihood is that about 14 more people
would be alive at 5-years compared to the existing SOC. Since about
210,000 advanced primary SCCHN patients globally would be eligible
for this treatment, the OS advantage seen in this study could mean
that about 29,000 more people would be alive at 5-years
post-therapy versus the SOC if all these patients received the
Multikine+CIZ treatment regimen followed by surgery and
radiotherapy.
By contrast, the SOC control group did not see any objective responses before surgery. CEL-SCI is
unaware of any existing therapy that provides complete or partial
tumor responses within three-weeks of treatment before surgery for
locally advanced primary SCCHN, much less objective responses
before surgery that are prognostic/predictive of longer survival,
as reached in this study.
It must be noted that Multikine is different from existing
therapies. Multikine is designed to be administered locally first,
immediately following diagnosis, to previously untreated patients whose tumors and any
involved lymph nodes are slated for surgical resection with
“intent-to-cure” SOC. To the company’s knowledge, there has been no
such therapy or neoadjuvant approved by FDA in at least several
decades for resectable locally advanced primary SCCHN. Although
existing checkpoint inhibitor drug therapies (like Keytruda) have
been approved and marketed as “first-line” treatments for head and
neck cancer, their indications are limited to the first-line
treatment of recurrent or non-resectable tumors. By contrast,
Multikine’s Proposed Indication would be for previously untreated,
locally advanced primary SCCHN patients scheduled for surgery and
radiation without chemotherapy, encompassing about 40% of the
entire advanced primary SCCHN population.
These Phase 3 trial results are intended to support a Biologics
Licensing Application to FDA, which has not yet been submitted. FDA
is the only U.S. entity authorized to determine safety and
efficacy, and Multikine is currently not approved.
About CEL-SCI Corporation
CEL-SCI believes that boosting a patient’s immune system while
it is still intact should provide the greatest possible impact on
survival. Therefore, in the Phase 3 study, CEL-SCI treated subjects
who were newly diagnosed with advanced primary squamous cell
carcinoma of the head and neck with the investigational product
Multikine first, before they received
surgery and radiotherapy, or surgery plus concurrent radiotherapy
and chemotherapy (the current standard of care for these patients).
This approach is unique. Most other cancer immunotherapies are
administered only after conventional therapies have been tried
and/or failed. Multikine (Leukocyte Interleukin, Injection)
received Orphan Drug designation from the FDA for neoadjuvant
therapy in patients with squamous cell carcinoma (cancer) of the
head and neck. CEL-SCI believes that this study is the largest
Phase 3 study in the world for the treatment of advanced primary
head and neck cancer.
Multikine is designed to help the immune system “see” the tumor
at a time when the immune system is still relatively intact and,
thereby, thought to be better able to mount an attack on the tumor.
The Phase 3 study was started in early 2011 and was fully enrolled
with 928 subjects in September 2016. To prove an overall survival
benefit, the study required CEL-SCI to wait until at least 298
(deaths) events had occurred among the two main comparator
groups.
The Company has operations in Vienna, Virginia, and in
Baltimore, Maryland.
Forward-Looking Statements
This press release contains forward-looking statements within
the meaning of Section 27A of the Securities Act of 1933, as
amended, and Section 21E of the Securities Exchange Act of 1934, as
amended. When used in this press release, the words "intends,"
"believes," "anticipated," "plans" and "expects," and similar
expressions, are intended to identify forward-looking statements.
Such statements are subject to risks and uncertainties that could
cause actual results to differ materially from those projected.
Such statements include, but are not limited to, statements about
the terms, expected proceeds, use of proceeds and closing of the
offering. Factors that could cause or contribute to such
differences include an inability to duplicate the clinical results
demonstrated in clinical studies, timely development of any
potential products that can be shown to be safe and effective,
receiving necessary regulatory approvals, difficulties in
manufacturing any of the Company's potential products, inability to
raise the necessary capital and the risk factors set forth from
time to time in CEL-SCI's filings with the Securities and Exchange
Commission, including but not limited to its report on Form 10-K
for the year ended September 30, 2021. The Company undertakes no
obligation to publicly release the result of any revision to these
forward-looking statements which may be made to reflect the events
or circumstances after the date hereof or to reflect the occurrence
of unanticipated events.
* Multikine (Leukocyte Interleukin, Injection) is the trademark
that CEL-SCI has registered for this investigational therapy. This
proprietary name is subject to FDA review in connection with the
Company's future anticipated regulatory submission for approval.
Multikine has not been licensed or approved for sale, barter or
exchange by the FDA or any other regulatory agency. Similarly, its
safety or efficacy has not been established for any use.
View source
version on businesswire.com: https://www.businesswire.com/news/home/20220818005806/en/
COMPANY: Gavin de Windt CEL-SCI Corporation (703) 506-9460
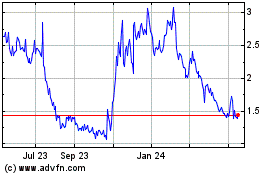
Cel Sci (AMEX:CVM)
Historical Stock Chart
From Apr 2024 to May 2024
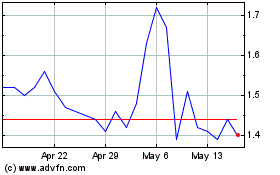
Cel Sci (AMEX:CVM)
Historical Stock Chart
From May 2023 to May 2024